
Voyages of Discovery Into New Media
At the crossroad of old journalism and new media, digital news entrepreneurs lead us on voyages of discovery into new media. From MinnPost to MediaStorm, these entities are using visual media, interactivity and social media to watchdog government abuse and the justice system, identify environmental dangers, and tell enduring stories. In doing so, they illuminate possibilities.
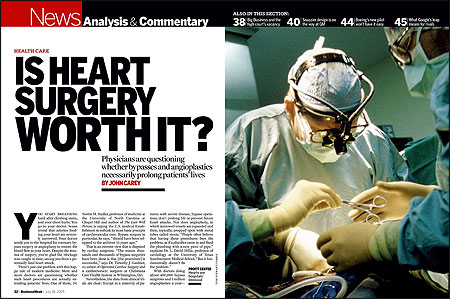
I didn’t set out to question the importance of lowering cholesterol, the subject of my BusinessWeek cover story “Do Cholesterol Drugs Do Any Good?” (January 28, 2008). Like most reporters, I had assumed that keeping “bad” (LDL) cholesterol in check is one of the most important steps people can take to stay healthy. So it was a surprise to pore over the actual clinical trials data and discover that the evidence is weaker than most people think.
Arriving at that conclusion, however, took a long time, with some outside nudges and lucky breaks. The initial seed was planted back in 2003 when Dr. Allen Roses, then a research vice president at GlaxoSmithKline, admitted the dirty little secret about drugs at a scientific meeting—that the large majority work only in a minority of people. I called my editor, Neil Gross, and said, “Wow, there’s got to be something big we can do on the lack of effectiveness of many drugs, now that industry itself has made this admission.”
Still, the idea percolated for several years, appearing occasionally as a factoid in smaller stories. Then Neil spotted another surprising medical assertion. Dr. Nortin Hadler, professor of medicine at the University of North Carolina at Chapel Hill, was claiming that heart bypass surgery is worthless and possibly barbaric. Look into it, he suggested. Preposterous, I thought. We’ve all heard so many stories of lives being saved by heart surgery. But the clinical evidence showed Hadler is right. We did a big takeout explaining how—and why—medical outcomes with bypass operations are usually no better than with other treatments, such as regimens of drugs, diet and exercise.
That story opened a wider door to the community of medical skeptics. I followed up with a cover story, “Medical Guesswork,” in May 2006 describing the weak evidence for the benefits of many medical procedures and treatments, from now-discredited tonsillectomies to spinal surgery.
The next year was taken up by other topics on my beat of covering science, technology, medicine, health and the environment from our Washington bureau. I did stories about food safety, climate change, and solar power, among others. But for our next medical project, Neil and I agreed, we needed to tackle the question of drug effectiveness. But how? The idea that drugs are not very effective was dismissed as being a story by one BusinessWeek editor: “Not surprising enough. Everyone knows that,” he told us.
Digging Into Data
But one reader of the “Medical Guesswork” story urged us to look at a statistic called “number needed to treat” or NNT. The NNT simply describes how many people have to take a drug for one person to benefit. I poked around and found that, yes, NNTs are surprisingly high even for many “good” drugs. Beta-blockers, for instance, are seen as essential in treating congestive heart failure. Yet 24 people must take them to prevent one hospitalization from heart failure (thus, an NNT of 24), and 40 people must take them to prevent one death (NNT of 40).
The poster child for this problem of high NNTs, I decided, is a diabetes drug called Avandia. The drug does a great job controlling blood sugar. But after reading stacks of scientific papers and having long conversations with critics like Hadler and Dr. Robert Ewart, professor of family medicine at the Southern Illinois University School of Medicine, I became convinced that the drug’s control of blood sugar doesn’t translate into anything clinically meaningful for diabetics, such as fewer heart attacks or kidney failures. Avandia’s NNT is close to infinite.
Along the way, I also learned the sobering lesson that you can’t trust the published conclusions in many scientific papers, because the conclusions are not supported by the actual data.
Avandia hit the headlines in May 2007 after a study linked the drug to a higher risk of heart attacks. I figured that we had our news peg. The press is missing the real story—the fact that the drug simply doesn’t work, I told Neil. I pitched a story focusing on Avandia and the concept of NNT but also mentioning that blockbuster cholesterol-lowering drugs like Lipitor don’t work all that well either, with NNTs over 100.
Could we sell the idea? The only people whose opinion really mattered were Editor in Chief Steve Adler and Executive Editor Ellen Pollock. I traveled up to New York from our Washington bureau to meet with them and Neil. They weren’t impressed with the tale of Avandia. Most readers wouldn’t have much interest in a diabetes drug, Steve said. But many of them are taking Lipitor or other cholesterol-lowering drugs in the same family of so-called statins, he observed. We could do a major public service—and make a big splash—by exposing the limitations of those drugs.
Examining Statins
Gulp, I thought. Knocking down Avandia would have been easy. Taking on the statins was much harder. After all, it was clear that statins do have benefits in people already at risk for heart disease, such as those who have suffered heart attacks or are diabetics. It would be a difficult and nuanced story, I told Adler. “No problem,” he said.
I wasn’t so sure, even as the stack of papers from medical journals rose on my desk. But, fortunately, the pieces began to fall in place. I found more and more doctors, researchers and patients who no longer worship at the altar of lowering LDL cholesterol. There was also compelling new research that offered an explanation for the conundrum of why statins help those at risk for heart disease while doing little for otherwise healthy people who have elevated LDL cholesterol levels. The research showed that, in addition to lowering cholesterol, the drugs have another biochemical effect. They reduce the inflammation that may help cause heart disease.
We also got help from an unexpected source, Lipitor’s maker, Pfizer. The giant drug maker started to run full-page ads touting the benefits of Lipitor for those not at high risk for heart disease. The ads said that in one key three-and-a-half year clinical trial, “three percent of patients taking a sugar pill or placebo had a heart attack compared to two percent of patients taking Lipitor.” Bingo, I thought. By Pfizer’s own admission, 100 people have to take the drug for more than three years for one to benefit, an NNT of 100. Everyone whose ears I bent about those numbers was surprised, especially considering that drug makers usually dismiss a 1 in 100 side effect as completely insignificant.
I wrote a draft. Then, with some trepidation, I asked Pfizer to comment on the story’s details. The company scheduled an interview with a top scientist, then canceled at the last minute, saying it would only respond in writing. When I finally got the response, I was surprised and gratified that it didn’t challenge our interpretations.
One mystery remained. Why hadn’t the story already been done? The fact that cholesterol-lowering statins are less effective than most people think wasn’t exactly new or deeply hidden. Top scientists had been making the case in scientific journals and other fora for years. But other than a few stories about cholesterol skeptics in the British press, the media had completely ignored the topic. The U.S. press seemed to accept as established truth that cholesterol lowering is vital and that statins are the closest thing to wonder drugs. I’m not any smarter than my colleagues, I worried. Maybe I’m just wrong.
The story sat on a shelf for a couple of weeks, while Neil and I fretted about what we might be missing. Then we had a stroke of luck. Results came out from a clinical trial called Enhance. Patients who were given both a statin and another drug that lowered their cholesterol further by a different mechanism showed no more benefit (on a measure of artery narrowing) than those given the statin alone. That was tantalizing evidence that cholesterol-lowering alone isn’t always important. We had our news peg. We rushed to add the Enhance results to the story and to get the story into the magazine that week. Then we braced for the response.
We need not have worried. The vast majority of letters and comments that poured in from doctors, journalists and ordinary people were positive. The story won the country’s top science writing award. I even heard later from people at Pfizer that company executives had wanted to write an angry rebuttal only to be told that there was nothing they could say because we got it right. And one of the story’s key conclusions, that doctors should largely ignore cholesterol and instead prescribe statins only to the smaller group of people at high risk for heart disease, was later supported by the results of a clinical trial, called JUPITER. The trial showed that people with high levels of inflammation (a key measure of risk) had fewer heart attacks while taking statins than those on placebo—even though they all had low levels of cholesterol to start.
The experience leaves me with a few simple-minded lessons. Question conventional wisdom. Examine the actual data in scientific papers rather than simply believe the conclusions or the press releases. Do the harder story, not the easy one. And work with great editors. Thanks, Neil and Steve.
John Carey is a senior correspondent in BusinessWeek’s Washington bureau who has covered science, technology, medicine, health and the environment since 1989. His reporting about statins was recognized with the 2008 AAAS Science Journalism Award for magazine reporting; he has also received awards from the Deadline Club, the American Institute of Biological Sciences, the Overseas Press Club, and the Aviation/Space Writers Association.
